Potential new oncology agents in England need to be approved by the National Institute for Health and Care Excellence (NICE) based on their cost-effectiveness. However over the past couple of years and much to the disappointment of the general public, NICE have rejected a string of oncology agents, including recently Kadcyla® for advanced breast cancer. Crown Bioscience review why so many drugs are failing to get approved and whether NICE guidelines need to be updated.
NICE is a non-departmental public body in England and Wales, responsible for appraising and producing guidelines on the use of new drugs. NICE base their guidance on efficacy and cost-effectiveness, and any drug they reject due to this will not be routinely available to patients via the National Health Service (NHS). In the past few years there has been a public outcry over NICE rejection of novel oncology agents, including most recently Kadcyla in advanced breast cancer. Kadcyla is an antibody-drug conjugate consisting of Herceptin® linked to the chemotherapeutic agent DM1 (a microtubule inhibitor). It is used to treat HER2 positive breast cancer following metastasis, which has stopped responding to all other treatments (including Herceptin alone) and which can’t be surgically removed. Kadcyla is unlikely to cause the side effects seen with standard chemotherapy, and could benefit 1,500 women a year in England. It was approved in the US in 2013 and reportedly more than 80% of US oncologists started prescribing the drug in its first 9 months on the market.
So, how does NICE make its recommendations on oncology drugs?
NICE uses quality-adjusted life years (QALY) to evaluate if a drug shows good cost-effectiveness. A QALY is defined by NICE as ‘A measure of the state of health of a person or group in which the benefits, in terms of length of life, are adjusted to reflect the quality of life. One QALY is equal to 1 year of life in perfect health’. Therefore a QALY is calculated by working out how many years of life a particular treatment will give to a patient, and adjusting this based on the quality of life per year. The normal threshold that NICE uses to approve drugs is an incremental cost-effectiveness ratio of £20,000 to £30,000 per QALY. This can be adjusted when the drug is an end-of-life cancer treatment allowing agents with a higher cost-effectiveness ratio to be approved. However, even as an end-of-life agent Kadcyla was estimated by NICE to have a cost-effectiveness ratio of £166,000 per QALY gained, which at over 5-times their regular upper threshold limit, NICE deemed too high for the drug to be approved.
Why are oncology drugs so expensive?
Most of the “easy” oncology drugs have now been discovered. The new therapies being developed are often second- or third-line treatments, and many are targeted agents which have taken a long time to develop for a small target population. As oncology agents only have a 5-10% success rate in the clinic, development costs for failed agents also need to be recouped via the drugs that do succeed. New agents which do pass clinical trials might also only add a few extra months of life for an advanced patient. For example, NICE reported that Kadcyla improved median overall survival by 5.8 months over the trial comparators lapatinib and capecitabine. While these 6 months are both scientifically significant and extremely important for the patients and their families, NICE feel they do not justify the price tag for £90,000 for a course of Kadcyla treatment. Drug companies can lower their prices (with Roche doing just this for Kadcyla) or offer access schemes to enable NICE approval; however, in this case NICE felt that this still did not justify approving the drug.
Is NICE right or should its policies change?
The debate now is whether the policy of NICE is correct for oncology drugs, or whether they need to change their thresholds. The NHS has a limited budget and cannot spend uncontrollably on expensive oncology drugs. However, the cost of oncology drug discovery and the development of new agents is not likely to drastically fall, and England cannot become a nation where all new oncology agents will never have a chance to be approved. Discussions on changing NICE thresholds and guidelines are likely to continue as drugs continue to be rejected.
In the meantime, women in England and Wales can apply for Kadcyla and other oncology agents not available through the NHS via the Cancer Drugs Fund. Over 200 women have received Kadcyla this way since April; however, the fund is due to end in 2016. Earlier this year the fund also announced that it is re-evaluating all of the drugs available from the fund to ensure that it is also as cost-effective as possible, which may mean some currently funded but expensive drugs may yet be removed.
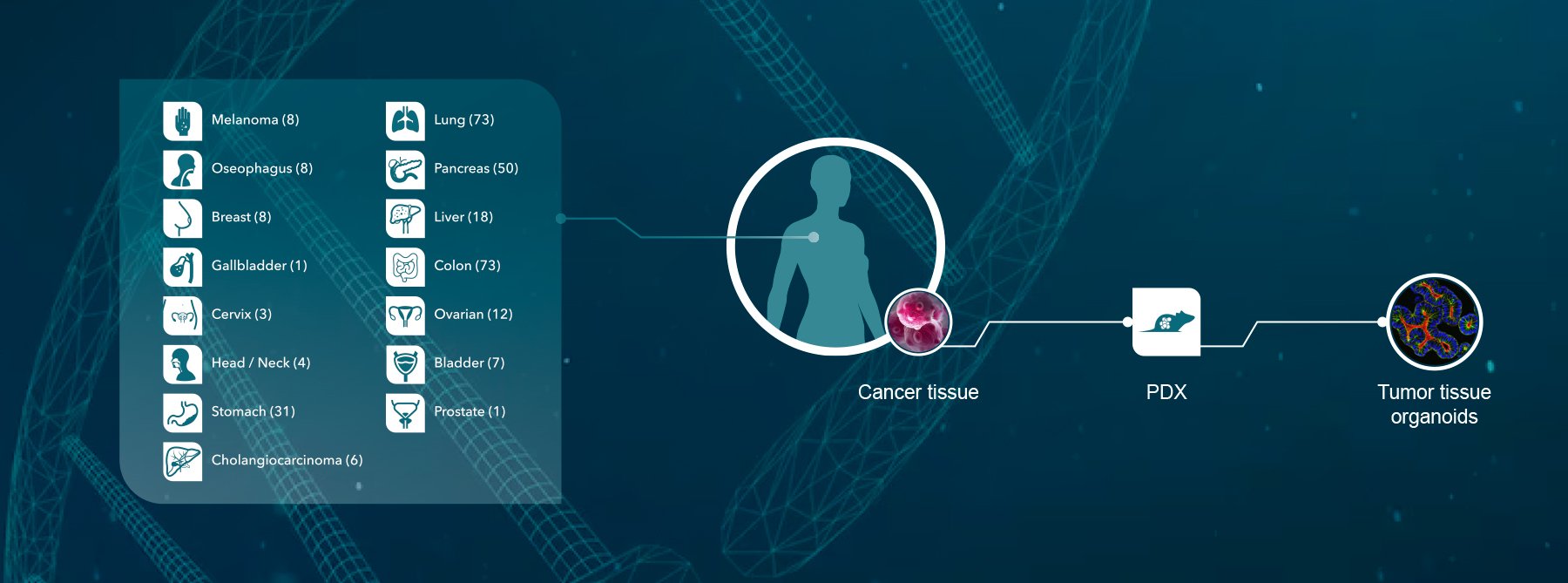
Crown Bioscience supports oncology drug discovery and the reduction of clinical trial failures and research costs with our pioneering preclinical Phase-II like human surrogate trials, HuTrials™. We utilize the world’s largest commercial collection of >1,100 genomically characterized patient-derived xenograft models (large enough to be truly reflective of the patient population) in our HuTrials. We can model responders and non-responders to identify a HuSignature™ from your results – a specific genetic signature which has a high correlation with drug response or drug resistance, and which can be used to identify patient populations with the best chance of clinical response to your agent. We also support research into advanced breast cancer with Herceptin resistant patient-derived xenograft models available. Contact us at busdev@crownbio.com to talk to our experts about how Crown Bioscience can meet your patient-derived xenograft research needs and how we can drive forward your oncology drug discovery projects today.