 We presented a wide range of immuno-oncology model data at AACR 2018, with three of our thirteen posters covering our novel murine homograft tumor models. Today, we’re reviewing the new data on KPC PDAC model development, a novel platform for QCing these models, and immunophenotyping to better understand change in model response.
We presented a wide range of immuno-oncology model data at AACR 2018, with three of our thirteen posters covering our novel murine homograft tumor models. Today, we’re reviewing the new data on KPC PDAC model development, a novel platform for QCing these models, and immunophenotyping to better understand change in model response.
AACR Poster 1144: Building Kras (G12D)/Trp53 null/Pdx1-cre (KPC) Mouse Homograft Tumor Models for the Efficacy Evaluation of Combinatory Immunotherapies
Effective treatments for pancreatic ductal adenocarcinoma (PDAC) are a current high unmet need. PDAC has a very poor five-year survival rate and few standard of care treatment options, with patients also being resistant to newer single agent anti-PD-1 and CTLA-4 immunotherapies. Researchers are now trying combinations of chemotherapies, small molecule immunomodulators, and immune checkpoint antibodies to treat this cancer, driving the need for relevant, immunocompetent models.
 KPC models (Kras (G12D)/Trp53 null/Pdx1-cre) are a good start, as they recapitulate human disease in morphology, immune microenvironment, and lack of treatment response. However, parental models are hard to use for pharmacology studies due to the spontaneous nature of tumor development, and they are expensive to breed.
KPC models (Kras (G12D)/Trp53 null/Pdx1-cre) are a good start, as they recapitulate human disease in morphology, immune microenvironment, and lack of treatment response. However, parental models are hard to use for pharmacology studies due to the spontaneous nature of tumor development, and they are expensive to breed.
Murine homograft tumor models can overcome these issues. They transplant spontaneous tumors from GEMM/carcinogen-induced models directly into immunocompetent mice, providing a murine version of PDX models. We’ve now developed a KPC murine homograft tumor model, and this poster details characterization and validation of the model for combination immunotherapy assessment.
KPC Murine Homograft Tumor Model Validated and Immunoprofiled
We validated a wide range of model features, first confirming that the homograft model histopathology is similar to both primary disease and mouse PDAC tumors, for both subcutaneous and orthotopic KPC homograft models, then profiling the subcutaneous and orthotopic tumors.
This immunoprofiling shows that the two models have similar immune environments to each other, with high levels of macrophages and low levels of effector CD4+ and CD8+ T cells. (Also nicely shown is a M1-M2 macrophage polarization).
The profiling also showed that the homograft tumors express low levels of PD-L1, which could potentially explain the poor response of this model to anti-PD-L1 treatment. Immunoprofiling post-treatment resembles vehicle-treated tumors (and tumors before treatment), consistent with the lack of response. Standard of care therapies are also assessed with the KPC model, with again both subcutaneous and orthotopic models being resistant to gemcitabine.
All of these factors mean that this KPC homograft recapitulates the primary disease’s lack of response to a range of therapies, providing a highly appropriate model for immunotherapy/combination immunotherapy assessment.
Our poster data further demonstrated the orthotopic homograft model responds to a novel immunotherapy, with increased survival.
Further Murine Homograft Tumor Models Available, with Mutational Load More Similar to Human Disease than Syngeneics
The poster also provides an overview of the overall murine tumor homograft platform, available models, and a comparison of mutation load with syngeneics; murine homograft models have a lower mutation load, providing a murine oncology model platform more comparable with human disease.
AACR 2018 Poster 5116: Development Of Murine Tumor Homograft Panels And Their Genetic Fingerprints For Identification, To Ensure Quality Controlled I/O Studies Using These Models
 With the increased use of mouse tumor homograft systems across immuno-oncology research, it’s prudent to track and QC the tumors to ensure correct ID. This isn’t as easy as for human-origin tumors (where genetic ID can be readily tracked by short tandem repeat genotyping or HLA typing) as murine tumors originate from limited strains of inbred experimental mice and lack markers for such quick and easy assays.
With the increased use of mouse tumor homograft systems across immuno-oncology research, it’s prudent to track and QC the tumors to ensure correct ID. This isn’t as easy as for human-origin tumors (where genetic ID can be readily tracked by short tandem repeat genotyping or HLA typing) as murine tumors originate from limited strains of inbred experimental mice and lack markers for such quick and easy assays.
In this poster, we detail the establishment of a novel, efficient model quality control and tumor ID method in murine tumor model systems, including homograft and syngeneic models. The assay is based on the genetic profiling of tumor models to identify unique genomic features that can be easily detected, such as gene fusions, for use as fingerprints for murine tumor model ID.
The assay process works like this:
- Original cell lines or mouse tumors are RNAseq’d to identify unique genetic features (gene fusions).
- RT-PCR and Sanger sequencing are then used to validate the presence of the same gene fusion in the tumor at passage 0.
- Subsequent test samples are also assessed for the same fusion.
- This confirms that the fusion is not lost and is a stable characteristic of the tumor that can be used as marker.
We validated the method for gene fusions in a murine homograft model and two syngeneic models, confirming this assay as a robust QC technique and that unique genetic features can serve as genetic fingerprints for murine model ID and quality control.
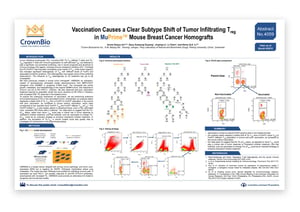
AACR 2018 Poster 4059: Vaccination Causes A Clear Subtype Shift Of Tumor Infiltrating Treg Cells In Mouse Breast Cancer Homografts
 Our final poster on murine homograft tumor models follows up on the mechanisms of action behind previously presented research. Way back at AACR 2016, we presented data on our mBR6004 breast cancer homograft model. This model was developed by orthotopic implantation of spontaneously developed breast adenocarcinoma from MMTV-PyVT transgenic mice into syngeneic FVB/N mice. The resulting model has similar growth, metastasis, and histopathology to the original GEMM tumors, and responds to CTLA-4, but not PD-1/PD-L1, inhibitors.
Our final poster on murine homograft tumor models follows up on the mechanisms of action behind previously presented research. Way back at AACR 2016, we presented data on our mBR6004 breast cancer homograft model. This model was developed by orthotopic implantation of spontaneously developed breast adenocarcinoma from MMTV-PyVT transgenic mice into syngeneic FVB/N mice. The resulting model has similar growth, metastasis, and histopathology to the original GEMM tumors, and responds to CTLA-4, but not PD-1/PD-L1, inhibitors.
Our AACR 2016 poster showed that vaccination makes the tumor responsive to PD-1/PD-L1 blockade, suggesting that host immune activation affects response to checkpoint inhibitors. Our new 2018 poster looks further into these data to reveal the background to this response.
Shift from FoxP3lo to FoxP3hi Population in Vaccinated Tumors
The poster briefly looks at how murine tumor homograft models are developed, the immune phenotype markers used, and the gating strategy behind the extensive phenotyping of tumor infiltrating lymphocytes (TIL) required to uncover the mechanism behind this new response.
FACS data show that, in tumors with prior vaccination, there is a drastic shift of TIL-Treg from a FoxP3lo to FoxP3hi population which probably corresponds to the previously published naïve FoxP3lo Treg and FoxP3hi effector Treg (eTreg). FoxP3 has long been considered a key marker of Treg, with recent research indicating significant heterogeneity of Treg with different levels of FoxP3 and associated functional variations. This supports reported conflicting roles of TIL in cancer prognosis and sensitivity to immuno-oncology agents.
Our poster suggests that the TIL-eTreg status, rather than naïve Treg, could play a critical role in tumor response to checkpoint inhibitor treatment. This could mean that methods such as prior vaccination to change the TIL-eTreg status could become an important strategy for enhancing checkpoint inhibitor treatment.
Look out for our other blog post summaries to catch up with all the latest AACR 2018 data on PDX, humanized models, ex vivo and in vitro assay platforms, and microbiome studies.